Links > Dry Skin TreatmentSkin Disorders And Their Treatment
Proper shingles treatment usually includes antiviral medication and vaccination for prevention. Although shingles can occur anywhere on your body, it most often appears as a single stripe of blisters that wraps around either the left or the right side of the torso. Also, contrary to what some people think of Shingles being an older person’s skin condition, I was 39 years old when I came down with a bout of Shingles. Prompt shingles treatment by your doctor is necessary to prevent it from spreading and to control the painful rash.
What Are Shingles?
Shingles are a viral infection that causes a painful body rash. The varicella-zoster virus – the same virus that causes chickenpox – is the cause of shingles. It’s also known as the Herpes-Zoster virus. After you’ve had chickenpox, the virus lies inactive in nerve tissue near your spinal cord and brain. Unfortunately, in later years, the virus may reactivate as shingles.
Most importantly, while it isn’t a life-threatening condition, shingles can be very painful. Vaccines can help reduce the risk of shingles, while early treatment can help shorten a shingles infection and lessen the chance of complications.
In brief, pain is usually the first symptom of shingles. For some, it can be very intense. Depending on the location of the pain, it can sometimes be mistaken for a symptom of problems affecting the heart, lungs, or kidneys. Also, some people experience shingles pain without ever developing the rash. Most commonly, the shingles rash develops as a stripe of blisters that wraps around either the left or right side of your torso. Sometimes the shingles rash occurs around one eye or on one side of the neck or face.
When To See A Doctor
Contact your doctor promptly if you suspect shingles, especially in the following situations:
- Pain and rashes occur near the eye. If left untreated, this infection can lead to permanent eye damage.
- You’re 60 or older because age significantly increases your risk of complications.
- You or someone in your family has a weakened immune system (due to cancer, medications, or chronic illness).
- The rash is widespread and painful.
Shingles Treatment – The Causes Of The Disease
As noted earlier, the varicella-zoster virus (Herpes-Zoster Virus) causes shingles. It is the same virus as your chickenpox outbreak when you were a child. Consequently, anyone who’s had chickenpox may develop shingles. After you recover from chickenpox, the virus can enter your nervous system and lie dormant for years. Eventually, it may reactivate and travel along nerve pathways to your skin — producing shingles. Fortunately, not everyone who’s had chickenpox will develop shingles.
The reason for shingles is unclear. But it may be due to lowered immunity to infections as you grow older. Shingles are more common in older adults and in people who have weakened immune systems.
Varicella-zoster is part of a group of viruses called herpes viruses, which include viruses that cause cold sores and genital herpes. Because of this, shingles are also known as herpes zoster. But the virus that causes chickenpox and shingles is not the same virus responsible for cold sores or genital herpes, a sexually transmitted infection.
Are You Contagious – Shingles Treatment
A person with shingles can pass on the varicella-zoster virus to anyone who isn’t immune to chickenpox. This usually occurs through direct contact with the open sores of the shingles rash. However, once infected, the person will develop chickenpox, not shingles.
Chickenpox can be dangerous for some people. Until your shingles blisters scab over, you are contagious and should avoid physical contact with anyone who hasn’t yet had chickenpox or the chickenpox vaccine. Also, this is equally true for people with weakened immune systems, expectant mothers, and newborn babies.
Risk Factors
Anyone who has ever had chickenpox can develop shingles. Most adults in the United States had chickenpox when they were children, before the advent of the routine childhood vaccination that now protects against chickenpox.
Factors That May Increase Your Risk Of Developing Shingles Include:
- Being older than 50. Shingles are most common in people older than 50. The risk increases with age. Some experts estimate that half the people aged 80 and older will have shingles.
- Having certain diseases. Diseases that weaken your immune system, such as HIV/AIDS and cancer, can increase your risk of shingles.
- Undergoing cancer treatments. Radiation or chemotherapy can lower your resistance to diseases and may trigger shingles.
- Taking certain medications. Drugs designed to prevent rejection of transplanted organs can increase your risk of shingles — as can prolong use of steroids, such as prednisone.
Complications Due To Shingles – Shingles Treatment
Complications From Shingles Can Include:
- Postherpetic neuralgia. For some people, shingles pain continues long after the blisters have cleared. The condition is also known as postherpetic neuralgia. It occurs when damaged nerve fibers send confusing and exaggerated messages of pain from your skin to your brain.
- Vision loss. Shingles in and around the eye (ophthalmic shingles) can cause painful eye infections that may result in vision loss.
- Neurological problems. Depending on which nerves are affected, shingles can cause inflammation of the brain (encephalitis), facial paralysis, or hearing or balance problems.
- Skin infections. If shingles blisters aren’t properly treated, bacterial skin infections may develop.
To Get A Good Moisturizer, Click On The Direct Link Here > https://www.anrdoezrs.net/click-8268793-13914692
Shingles Treatment – Prevention
Two vaccines may help prevent shingles, namely the chickenpox (varicella) vaccine, and the shingles (varicella-zoster) vaccine.
Chickenpox Vaccine
The varicella vaccine (Varivax) has become a routine childhood immunization to prevent chickenpox. The vaccine is also recommended for adults who’ve never had chickenpox. In short, though the vaccine doesn’t guarantee you won’t get chickenpox or shingles, it can reduce your chances of complications and reduce the severity of the disease.
Shingles Vaccine
People looking to receive the shingles vaccine have two options: Zostavax and Shingrix.
Zostavax was approved by the Food and Drug Administration (FDA) in 2006. It has been shown to offer protection against shingles for about five years. In addition, it’s a live vaccine given as a single injection, usually in the upper arm.
Shingrix was approved by the FDA in 2017 and is the preferred alternative to Zostavax. Studies suggest Shingrix also offers protection against shingles beyond five years. It’s a nonliving vaccine made of a virus component. It is given in two doses, with two to six months between doses.
Furthermore, Shingrix is approved and recommended for people aged 50 and older, including those who’ve previously received Zostavax. Zostavax isn’t recommended until age 60.
In short, the most common side effects of either shingles vaccine are redness, pain, tenderness, swelling and itching at the injection site, and headaches.
****** As with the chickenpox vaccine, the shingles vaccine doesn’t guarantee you won’t get shingles. However, this vaccine will likely reduce the course and severity of the disease and reduce your risk of postherpetic neuralgia. ******
Personal Note: The shingles vaccine is only a prevention strategy. Also, it is not for treating people who currently have the disease. Talk to your doctor about which option is right for you.
Diagnosis is usually done by physical examination and review of medical history.
Common Tests and Procedures
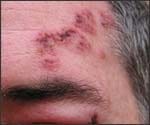
Physical examination: Physical examination of rashes and blisters is adequate to make a diagnosis.
Varicella-zoster virus tests: In rare cases, fluid from the blisters is tested to confirm the presence of the virus.
Shingles Treatment – Symptoms
It Can Have the Following Symptoms:
- Headache
- Fever and chills
- Malaise
- Nausea
- Body aches
- Swollen lymph glands
- Burning, itching, or tingling sensation
- Red patches
- Fluid-filled blisters that break easily
- Rash on the face and ears
- Itching
- Muscle weakness
- Fatigue
- Stomach upset
Shingles Treatment Usually Includes Medication and Vaccination for Prevention.
Medications
Antivirals: These drugs will kill the virus or suppress its ability to replicate.
Acyclovir
Valacyclovir
Famciclovir
Anti-inflammatory Drugs: These drugs will manage inflammation due to the infected virus.
Ibuprofen
Diphenhydramine
Capsaicin
Aside from shingles, Allies of Skin has some great anti-wrinkle skin care products that can give you firmer, youthful-looking skin. Do take a look at what Allies of Skin has to offer on its Online Store.
Therefore, to check out these great products today, click on the direct link here > https://www.anrdoezrs.net/click-8268793-13914692
Medical Note: Should you or a family member come down with Shingles, contact your doctor right away to avoid spreading the disease and to limit whatever pain you might have. Also, do not try to self-medicate Shingles. Your doctor can prescribe the best treatment for you!